They have also been shown to incorporate into neovessels at sites of ischemia. These cells have been termed “endothelial progenitor cells” (EPCs) and express various endothelial cell markers. This concept was overturned by Asahara and colleagues, who published that purified CD34 + hematopoietic progenitor cells can differentiate into endothelial cells ex vivo. New blood vessel growth (neovascularization), however, is a process currently being re-evaluated in light of recent advances in progenitor cell biology. This process is also called vasculogenesis. The differentiation of mesodermal cells into angioblasts, cells that subsequently differentiate into endothelial cells, is believed to exclusively occur during embryonic development. Angiogenesis is the process of forming new blood vessels from pre-existing ones. Endothelial cells are a critical component of neovascularization and form new blood vessels through both the angiogenesis and vasculogenesis processes. Neovascularization includes angiogenesis and vasculo-genesis. Burn blisters contain many growth factors, and therefore may be responsible for the neovascularization of burn wound healing. Although neovascularization plays a crucial role in burn wound healing, the effect of burn blister fluids on neovascularization has not been fully explored. In addition, these studies have demonstrated the detrimental aspects of blister debridement, whereby removing blisters causes a loss of the antioxidative burn blister fluid while also decreasing the circulation in an already compromised wound. These studies have shown that blisters have a stimulatory effect on wound healing due to the presence of various growth factors, while also facilitating fibroblast growth. The in vivo and in vitro studies that have been published regarding blister management vary in their results. 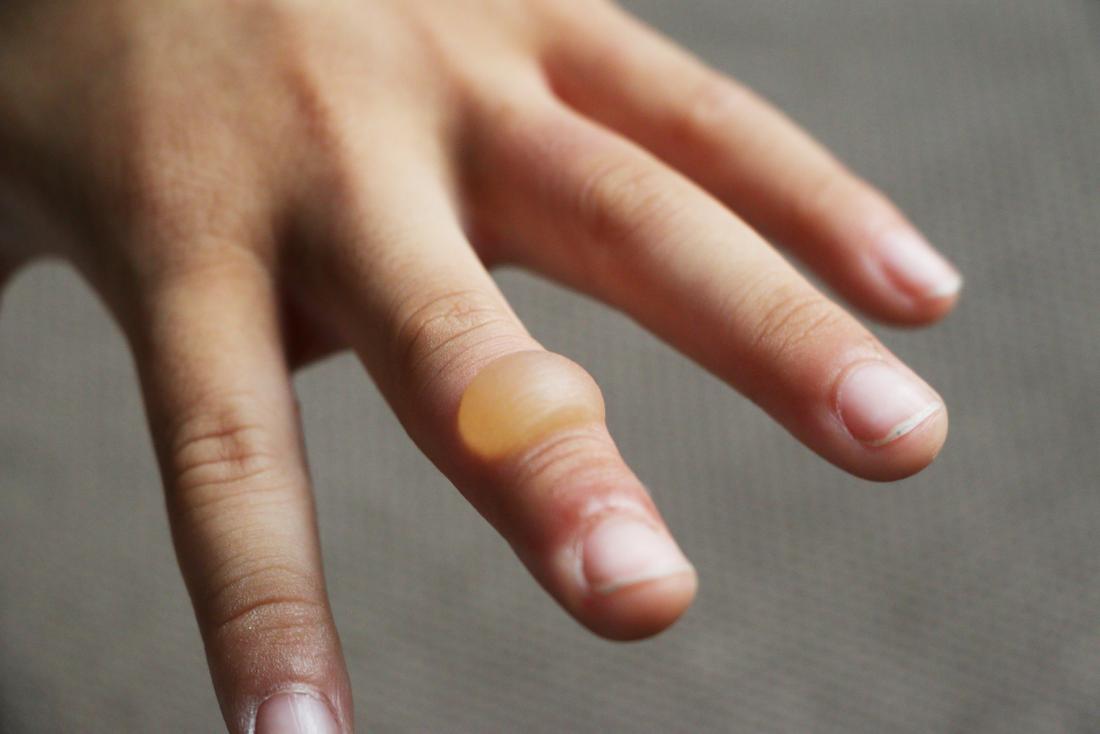
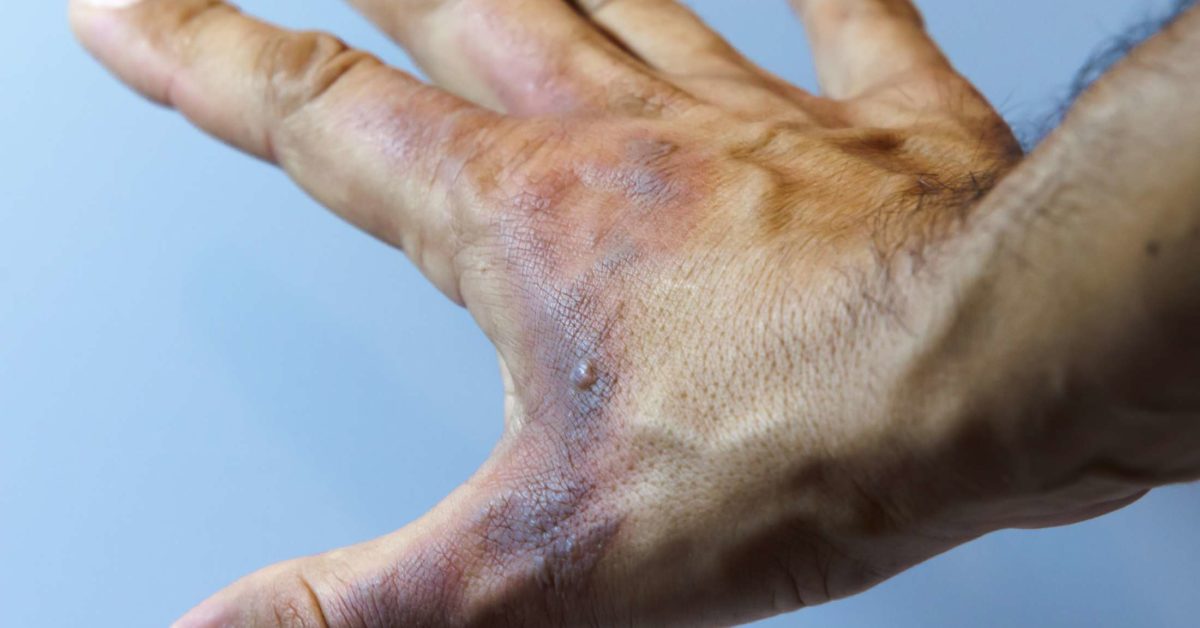
Burn blisters, which are formed as a result of inflammatory changes in the early burn injury, are a physiological response that increases capillary permeability to allow for edema formation between the epidermis and the dermis. Therefore, if the wound is not healed in 3 weeks, wound debridement and grafting is necessary.īlistering may occur as a secondary event associated with a burn injury and they are found in both SPTB and DPTB wounds. Due to prolongation in the inflammatory and proliferative phases, wound closure is delayed, which leads to skin scarring and contracture. Even if no infection occurs following injury, DPTB wounds still need longer than 3 weeks to heal. Due to the destruction of the epithelial cells in the skin appendages, reepithelialization in these wounds is greatly retarded. It is therefore often difficult to distinguish between SPTB and DPTB wounds. Skin blisters are still present, however, making it difficult to determine the burn depth of the wound. In addition, the heat from the burn kills the nerve endings, thus making the wound relatively insensate. These burns are typically dry and mottled pink or white in appearance. In contrast to SPTB wounds, DPTB wounds involve an injury to the full thickness of the epidermis and the reticular portion of the dermis. Unless complications occur, the optimal treatment for these wounds is to support them with regular dressing changes. This type of injury usually has a zone of stasis and may convert to a much deeper wound, however, if the treatment is inappropriate. This is especially known to occur in people of Asian descent. These burns generally heal within 2 weeks, and relatively little scarring occurs however, the injured skin may result in a color change due to hyperpigmentation. Healing occurs rapidly following SPTB injury, whereby the wound quickly becomes completely reepithelialized by the migration of epithelial cells from the deeper portion of the hair follicles, as well as from the sweat and sebaceous glands to the wound site. In addition, skin blisters are often present at the injured area. These lesions are typically pink, moist, and very painful due to the sparing damage of the nerve endings in the mid-dermis. In SPTB injury, the whole layer of the epidermis is destroyed, as are various portions of the dermis. Superficial partial-thickness burns (SPTB) and deep partial-thickness burns (DPTB) differ in their appearance, ability to heal, and the potential need for debridement and skin grafting. Second-degree burns are partial-thickness by definition, but they can be further categorized as either a superficial or a deep burn. 
0 Comments
Leave a Reply. |

 RSS Feed
RSS Feed
